For the millions of Americans suffering from depression, anxiety and PTSD, alternative treatments can help
The data is overwhelmingly clear: today’s mental health landscape is concerning — especially for the nearly 53 million Americans with a mental health condition. According to Tracy Dennis-Tiwary, PhD, professor of psychology and neuroscience at Hunter College, half of us will be clinically diagnosed with a mental illness in our lifetime. What’s more? The annual suicide rate in the U.S. increased 30% between 2000 and 2020.
For decades, the most prescribed answer to the rising mental health pandemic in the U.S. (and, increasingly, around the world) has been psychopharmaceuticals, which alter the mental state of their user. It’s true that these drugs, especially when combined with therapy, have helped people better manage their behavioral health. However, there is still so much we don’t know about mental health disorders — what causes them, how to best treat them, who benefits from antidepressant medications. What we do know is that while psychopharmaceuticals have become a multi-billion dollar per year industry in the U.S., their widespread efficacy is questionable at best.
More than ever — and on the heels of a 25% global increase in the prevalence of anxiety and depression due to the COVID-19 pandemic — there is a critical need for alternative treatment methods to support the millions of Americans who don’t benefit from antidepressants and other medications. Continue reading to learn more about the downfalls of commonly prescribed drugs like selective serotonin reuptake inhibitors (SSRIs) and the rise of ketamine therapy, which can provide both immediate relief and long-term improvements in mental health management.
Do antidepressants work?
Navigating the ups and downs of treating a mood disorder isn’t easy. In fact, as many as 30% of people who take antidepressants do not experience relief from their symptoms. And even when those medications work, patients usually develop resistance or build up tolerance — which requires them to take a higher dose, switch to a new drug, or add an additional medication to their regimen.
There are also plenty of undesirable side effects — emotional numbing, decreased libido, agitation, sleep disturbances, weight gain and even suicidal thoughts. According to The New York Times, 15.5 million Americans have been taking psychopharmaceuticals for at least five years, a rate that has more than tripled since 2000.

These drugs were initially approved for short-term use — and we have limited data about what happens when people take them indefinitely.
Additionally, little guidance exists for those who want to stop taking antidepressants, which comes with its own set of short- and long-term withdrawal symptoms (weight gain, anxiety and nausea are some of the most common).
While there is much to debate around the mainstream use of psychopharmaceuticals — including allegations that pharmaceutical companies exaggerate claims of drug efficacy and downplay the health risks of antidepressant use in consumer advertising — it’s clear that these drugs are not a one-size-fits-all solution. Dr. David Katz, founding director of the prevention research center at Yale University’s Griffin Hospital, said that “antidepressant drugs tend to be only nominally effective, even in the short term,” and much of their impact is due to the nonmedicinal placebo effect.
So, for the millions of Americans who take antidepressants and don’t experience relief from their symptoms, what’s the solution?
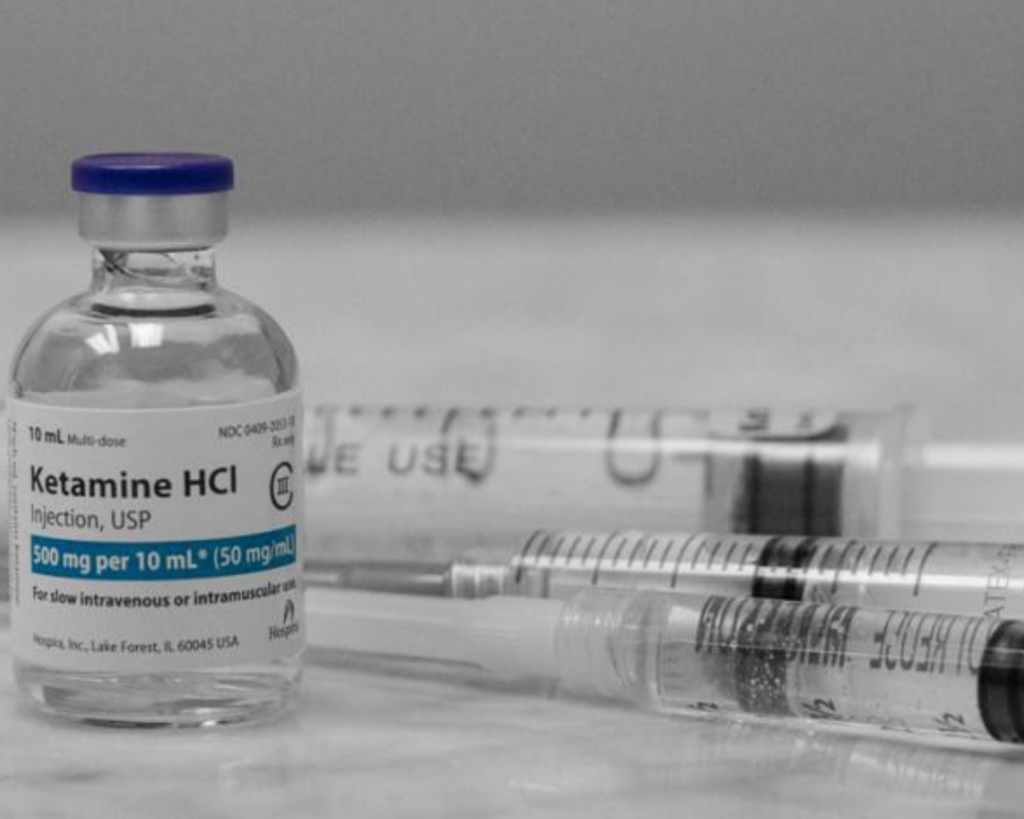
The increasing popularity of ketamine
As the science of traditional treatment methods continues to come into question, we’re seeing a rise in the use of other medications that might work better. Ketamine, for example, is an FDA-approved drug that has been safely used as an anesthetic since the 1970s. Most recently, though, it has gained popularity for its use in improving treatment-resistant mental health disorders, PTSD and chronic pain more quickly and effectively than other medications through a different mechanism of action.
John Krystal, MD, chief psychiatrist at Yale Medicine, has been researching ketamine as a treatment for depression since the 1990s. He found that “ketamine triggers reactions in [the] cortex that enable brain connections to regrow,” creating a lasting anti-anxiety effect. Krystal and a team at Yale School of Medicine also found that a single subanesthetic dose of ketamine improved depression and in some cases “led to a near-complete recovery” in less than 24 hours. It has also been shown to quickly reduce suicidality.
In 2006, the National Institute of Mental Health concluded that a single intravenous dose of ketamine had rapid antidepressant effects.
Prescribing ketamine for depression and other disorders
As of 2022, following the influx of success stories about patients trying ketamine infusions to treat depression, hundreds of ketamine clinics have popped up across the U.S. But there are also direct-to-home ketamine subscription kits that consumers should be wary of. Physician-administered low-dose intravenous (IV) ketamine infusions are the preferred method for most effectively administering the drug to patients. During these controlled infusions, ketamine releases growth factors that establish new connections and interrupt negative thought patterns in the brain.
Unlike with antidepressants, those treated with ketamine do not build up resistance to it over the course of treatment and beyond. While patients taking antidepressants — which typically take weeks to build up in a patient’s system — are often required to be on them for the long term, most patients need just six weekly ketamine infusions to feel lasting relief from their symptoms.
Ketamine’s key benefits
- Provides immediate relief from symptoms of depression, anxiety, PTSD and chronic pain, while SSRIs can take between four and 12 weeks to work.
- Virtually no short- or long-term side effects when administered by a licensed physician. Some people might experience a mild increase in blood pressure and heart rate during infusions, which is safely managed in a clinical setting.
- Can eliminate the need for antidepressants.
- Proven safe and effective.
- High rate of success.

A better, brighter future for mental health
Mental health disorders are not going anywhere — and the need for safe and effective treatment methods for those who suffer from them will only increase. While some people do respond to psychopharmaceuticals like antidepressants and anti-anxiety medications, they aren’t for everyone, and we still don’t know if they’re an acceptable long-term solution. As more and more science-backed studies and data continue to support it, the use of ketamine for treatment-resistant mood disorders offers much-needed hope for those who haven’t yet found relief.
The ketamine treatment process: What to look for
If you’re considering ketamine as a treatment for a mood disorder, it’s important to find a credentialed clinic that combines physician-administered IV ketamine infusions with psychotherapy for optimal results. Additionally, ketamine is not for everyone, so your clinic should offer a comprehensive screening process before prescribing it.
At NeoMedicine Institute, we offer a five-step treatment process during which our clinicians are with our patients every step of the way:
- Consultation: New patients meet with our doctors for a comprehensive evaluation in which we determine if ketamine is right for you and customize a treatment plan.
- Infusion therapy: Patients receive up to six ketamine infusions lasting 40-90 minutes each, under close supervision, safely administered by our doctors.
- Psychotherapy: Before, during and after treatment, patients meet with an in-house psychologist.
- Follow up: Our team checks in with each patient throughout treatment to answer questions, chart progress and make adjustments.
- Maintenance program: If needed, we offer an FDA-approved ketamine nasal spray (called esketamine) maintenance program to sustain results.
If you’re interested in learning more about our ketamine treatment program, contact NeoMedicine Institute.